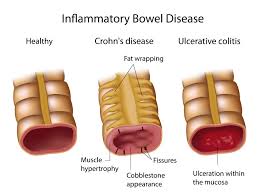
Crohn’s Disease & Ulcerative Colitis
Crohn's disease is a type of inflammatory bowel disease (IBD). It causes swelling of the tissues (inflammation) in your digestive tract.

Crohn’s Disease & Ulcerative Colitis
Crohn’s disease and Ulcerative colitis are both inflammatory conditions of the GI tract. Crohn’s disease affects the entirety of bowel (small and large intestine) and the entire thickness of the bowel. Ulcerative colitis is limited to the large intestine and affects the inner lining only. Both diseases are autoimmune diseases where the body attacks itself. These diseases can cause significant life distress requiring many doctor visits, medications and decreased quality of life.
Did you know?
Abdominal pain is the most common symptom of Crohn’s disease, but exactly where that pain occurs depends on which area of the digestive tract is affected.
Symptoms of Crohn’s Disease & Ulcerative Colitis
- Abdominal pain and cramping
- Diarhea that is sometimes bloody (colitis)
- Rectal bleeding (colitis)
- Bloating
- Fever (during acute attack)
- Nausea
- Vomiting
- Weight loss
- Fatigue
- Anxiety
Frequently Asked Questions (FAQ) - Crohn’s Disease & Ulcerative Colitis
What is causing my ulcerative colitis and crohns disease?
UC and Crohn’s can be brought on by poor diet, medication use, stress, etc leading to dysbiosis or bacterial imbalance and pathogenic overgrowth in the GI tract as well inadequate digestion and absorption of food and impaired motility of the GI tract. This can all lead to impaired detoxification in the body and increased total toxic burden leading to systemic inflammation.
What are typical treatments for ulcerative colitis and crohns disease?
Typical treatments are aimed at treating the immediate symptom with medications like immune modulators that basically suppress the immune system and Aminosalicylates to reduce inflammation. These medications will make the symptoms better with their use but do not address the cause leading to dependency on the medication and frequent dosage changes.
How do I figure out what is causing my ulcerative colitis and crohns disease?
Getting a comprehensive stool analysis will allow your practitioner to see exactly what is going on inside of your GI tract I.e. bacterial balance, digestion and absorption markers, pathogenic overgrowth, and inflammation. Also, thinking about toxin overload as a potential contributor and trigger to this condition. This will allow for a customized treatment plan to be developed based on your symptoms, history and biomarker analysis. Addressing lifestyle factors such as diet, exercise, sleep, and stress management are also important aspects to a comprehensive treatment plan.